CAN BONES CHANGE SHAPE FROM SUSTAINED PRESSURE OR LOADING?
How do bones grow in length an width? What exactly makes them grow?
During intense physical activities like running or jumping, your bones quietly redesign themselves.
This hidden transformation is called bone modeling.[1]
This article explains what bone modeling is, and how it contributes to bone transformation or growth.
Before getting into how bone models or transforms, it helps to understand what exactly bone is made of.
What Is Bone Made Of?
Bone is a solid material built from three primary components:
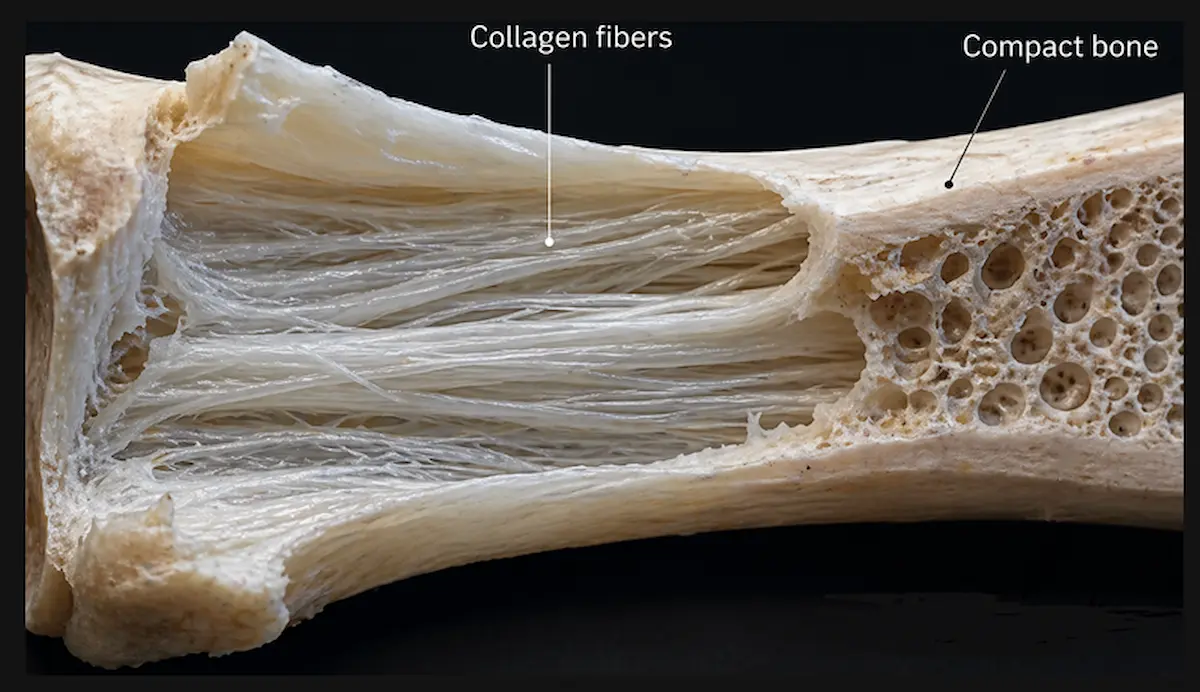
1. The Collagen Framework
About one third of bone’s weight is an organic matrix built primarily from type I collagen, the same protein found in tendons and ligaments.
Collagen gives bone its flexibility and tensile strength.
It is what prevents bone from being brittle.[2]
When a force is applied, the collagen fibres allow the bone to flex very slightly rather than snap.
Just like the steel reinforcement inside a concrete structure.
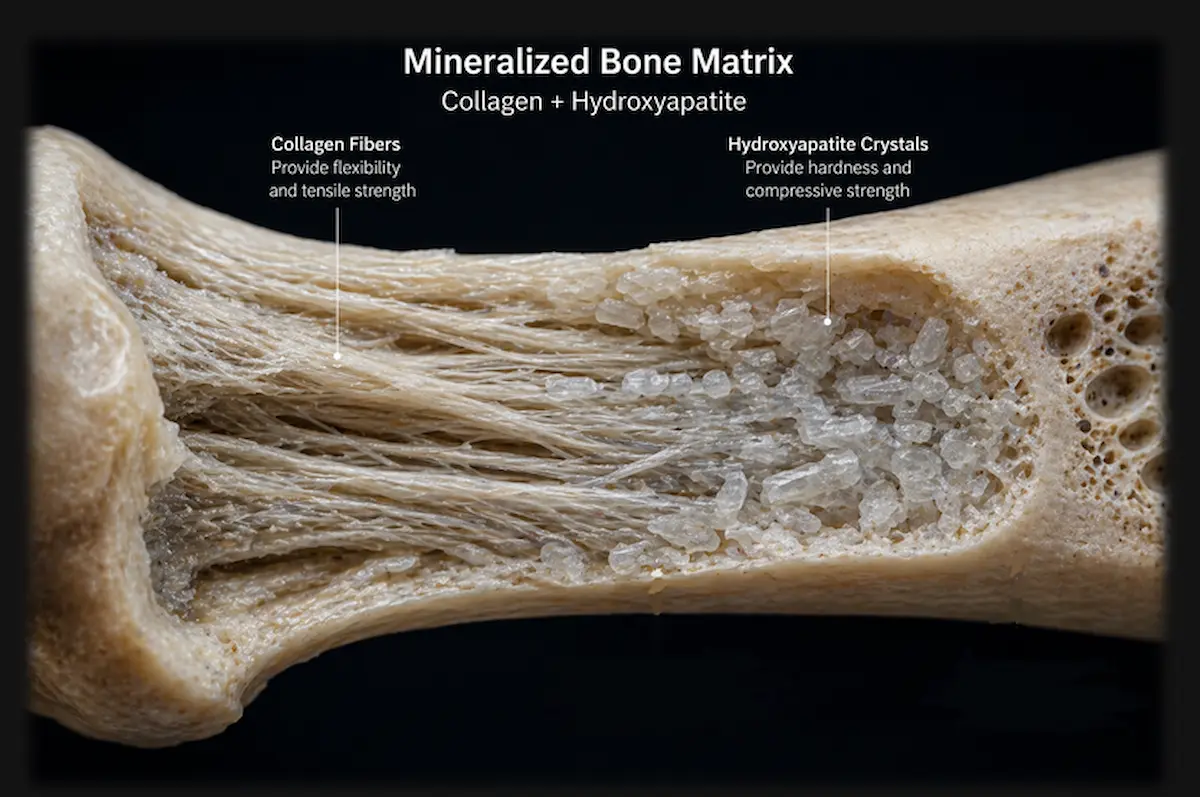
2. The Mineral Component
The remaining two thirds of bone are minerals , particularly hydroxyapatite, a crystalline form of calcium phosphate.
Hydroxyapatite crystals are deposited within and around the collagen framework to give bone its firmness and ability to resist any external forces.
The combination of these two materials is what makes bone exceptional: tough enough to resist tension, hard enough to resist compression, structured in a way that transmits mechanical signals directly to the cells living within the matrix.
It also contains proteins, lipids, and four specialized cell types that manage every stage of bone construction and renewal.
The collagen matrix is what gives bone its flexibility and tensile strength , its ability to bend slightly under load without shattering.
Proteins embedded in the matrix regulate its mineralization and reinforce its collagen architecture.
When this system is healthy and well-loaded, the result is bone that is both strong and structurally adaptable.
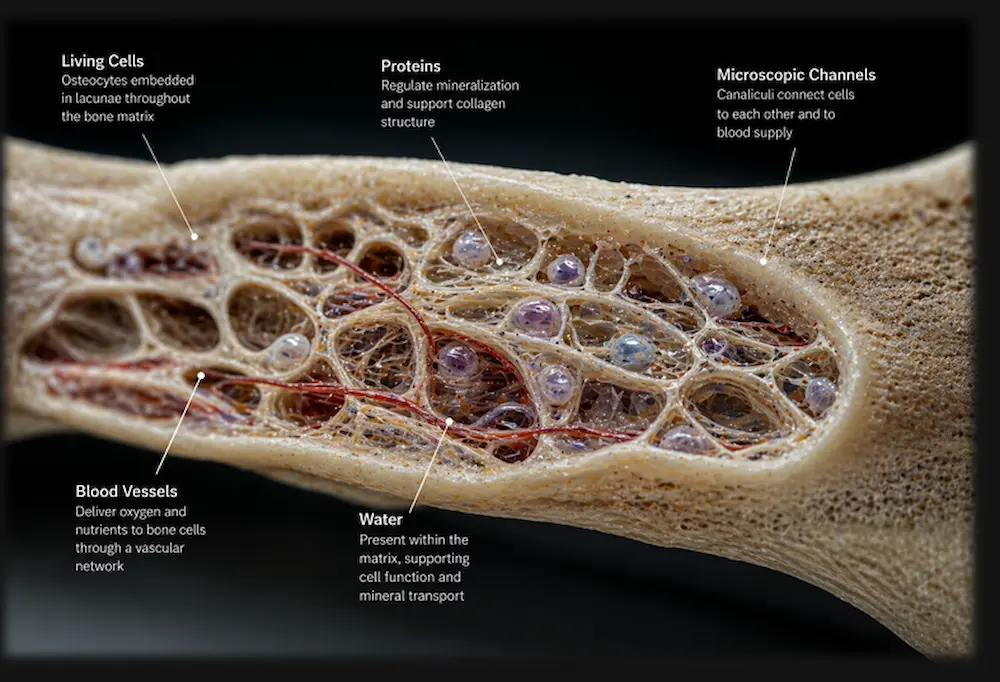
3.The Living Cells Inside the Matrix
Bone also contains water, and proteins which regulate mineralization, but most importantly, it contains living cells embedded throughout the structure.
Hence, bone is not a static deposit of calcium, rather it is as biologically active as muscle, skin, or any other tissue and like those tissues, it responds to the demands placed on it.
What is bone modeling ?
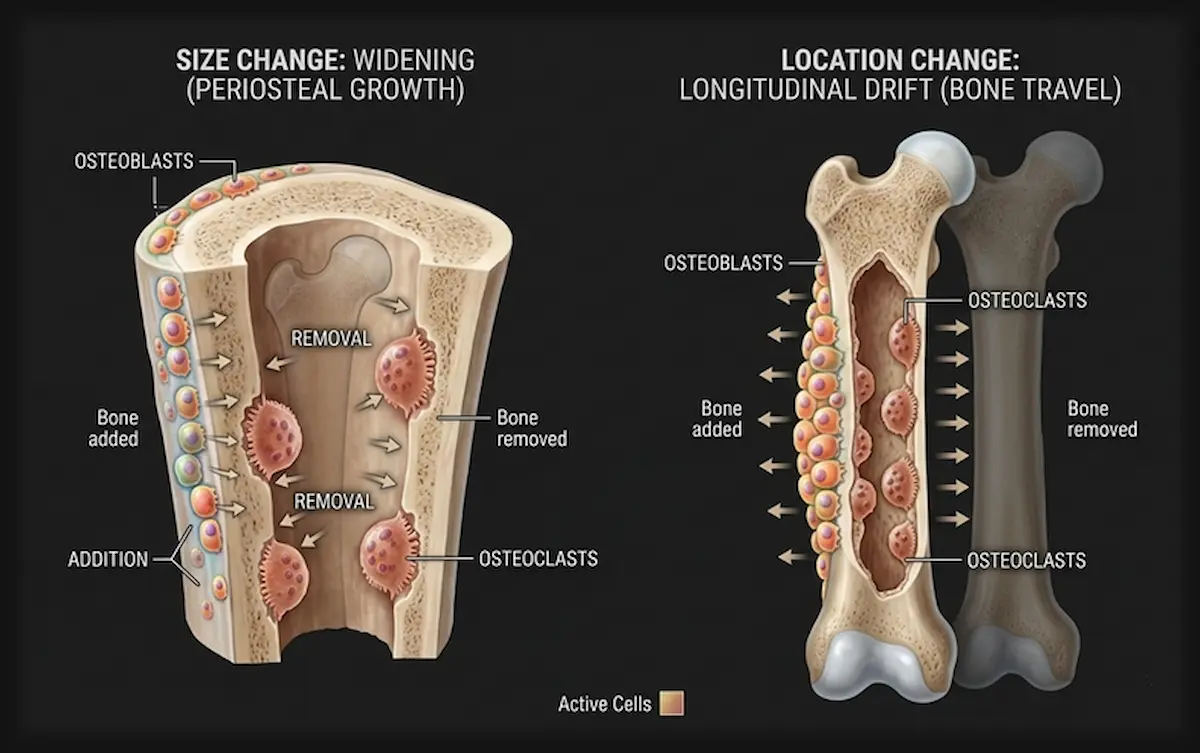
Bone modelling is the process by which bones change shape or size in response to physiologic influences or mechanical forces that are encountered by the skeleton like exercises.[3]
Unlike remodeling (which mostly recycles bone in the same spot), modeling molds the bone into a new form; thicker, straighter, or better aligned with the forces acting on it.
It is not about repairing damage or renewing old tissue.
It is about structural change.
The defining characteristic of modeling is this:
osteoblasts and osteoclasts work at different sites simultaneously.
Bone is being removed from one surface while new bone is being deposited on another.
The structure shifts wider here, narrower there, straighter, denser, differently proportioned , without losing its integrity at any point in the process.
The Cells That Control the Modeling Process
Three specialized cell types manage bone throughout life.
Each plays a distinct role, and their coordination is what allows bone to respond intelligently to mechanical input.
Cell 01
Osteoblasts — The Builders
These are the cells responsible for the manufacture and mineralization of new bone.
The process of bone formation begins with the osteoblasts manufacturing a protein matrix or mixture ( Osteoid ) which is made up of mainly collagen and other organic proteins.
Once the matrix is laid down, they mineralize it by depositing calcium and phosphorus, hardening it into solid bone.
Growth hormone release is one of the primary triggers for osteoid production.
After completing their work, osteoblasts either die, flatten into bone-lining cells, or get buried within the matrix and transition into osteocytes. [4]
Cell 02
Osteocytes — The Sensors
Osteocytes are simply osteoblasts that are no longer active. They form when osteoblasts become buried in the mineral matrix of bone.
They coordinate the actions of osteoblasts and osteoclasts via several mechanisms.
For instance, they squeeze out and release proteins that signal to osteoblasts, osteoclasts, and other bone-residing cells to respond to environmental changes.
Hence, they act as sensors when stress is applied to bones or in case of bone fractures, signaling osteoclasts to dissolve the bone.
Cell 03
Osteoclasts — The Demolition Crew
The cells responsible for dissolving or breaking down old bones.
They achieve this by secreting an acid that destroys the bone matrix.
This role played by osteoclasts is very vital for bone remodeling which involves continuously removing and replacing bone tissue for structured growth and in response to mechanical stress applied to bones.[5]
Cell 04
Chondrocytes — The Cartilage Cells
Chondrocytes are the cells found in cartilage, play a vital role of repairing cartilage, and act as a template for bone growth when bones are still lengthening.
The key relationship:
Osteoblasts and osteoclasts do not work independently.
They communicate through a tightly regulated system of chemical signals known as coupling.
The balance between their activity at any given location on bone determines whether bone is gained, lost, or redistributed there and that balance is directly influenced by the mechanical forces the bone experiences.
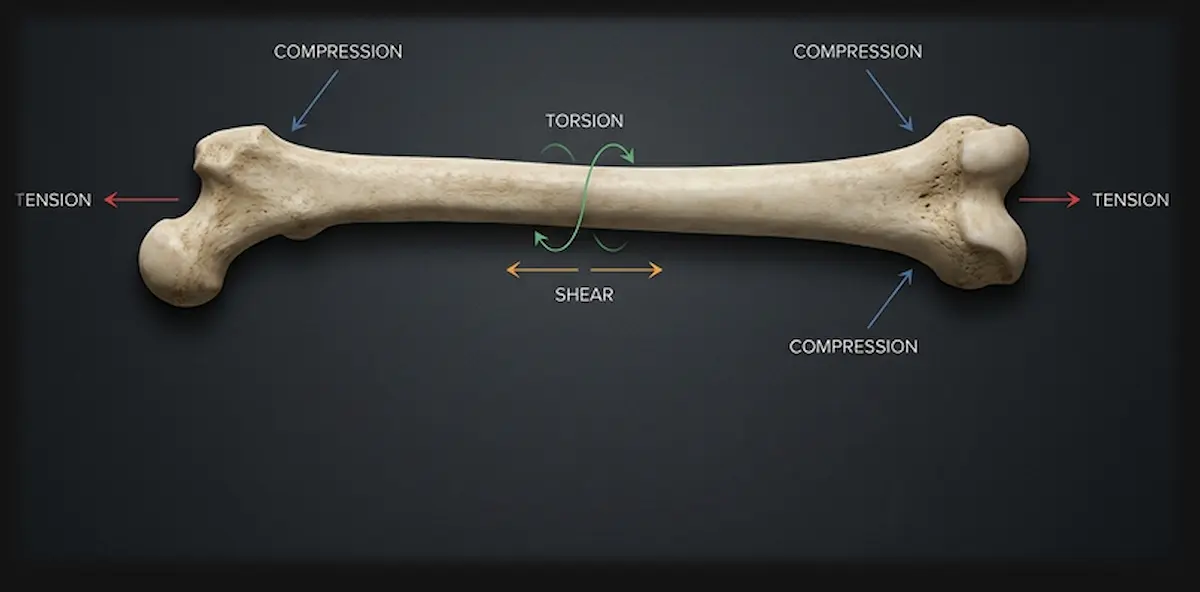
The Four Forces Acting on Bone
Every time you move, multiple mechanical forces act on your bones simultaneously.
Understanding what those forces are is the starting point for understanding why bone changes the way it does in response to physical activity.
Every physical movement generates a combination of these forces at different points along the skeleton.
A runner’s tibia experiences compression (body weight pressing down), tension (the bone flexing under load), torsion (slight twisting with each stride), and shear (forces acting diagonally across the shaft) often all at once.
What matters for bone modeling is which of these forces the bone experiences consistently, at what magnitude, and from which direction.
The cells inside bone , particularly the osteocytes detect these forces and translate them into biological instructions that tell other cells where to build and where to remove bone tissue.[6]
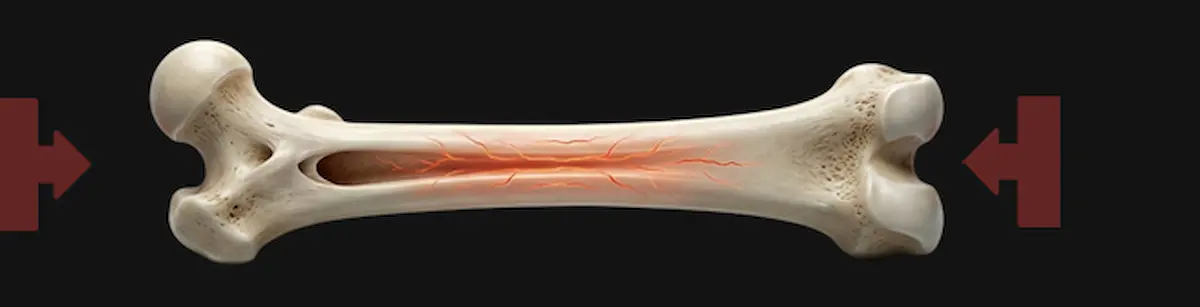
1. Compression
Compression forces are the pushing or squeezing forces that act on bone.
Take an example of what happens when you are standing.
Your leg bone are constantly supporting your entire body weight.
The same applies to jumping or running.
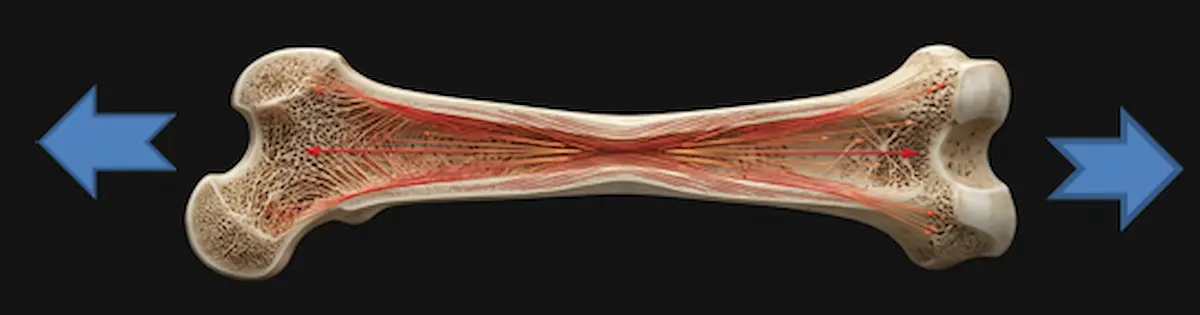
2. Tension force
Tension on bone that pulls the matrix apart acts as a key mechanical signal stimulating periosteal bone deposition (the outer membrane of the bone), which drives appositional growth.[7]
This process is part of the body’s adaptive response to mechanical stress, where tension often promotes bone formation on the periosteal surface [8]
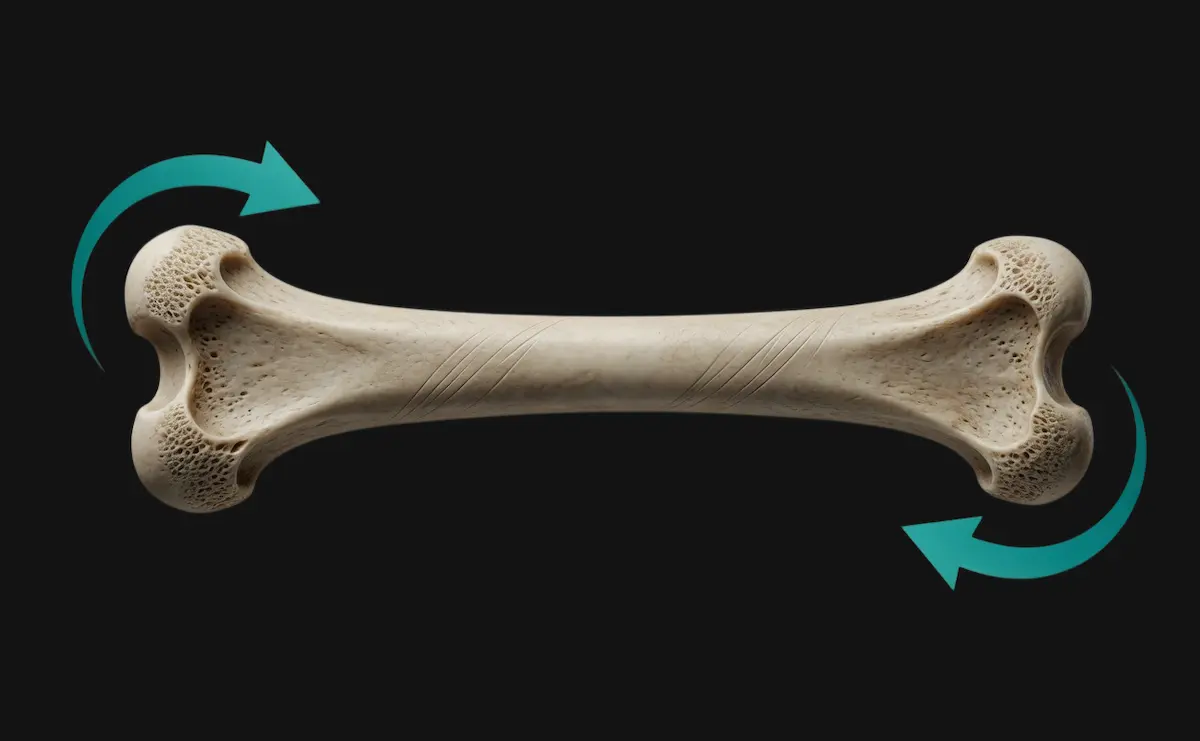
3. Torsion
Twists bone around its long axis sometimes causing spiral fractures.
For instance; when a football player plants their foot, and the body rotates, creating a twist in the tibia.
4. Shear
Applies force diagonally across the bone structure.
Influences cross-sectional shape over time; creates asymmetric loading signals.
How Force Reshapes Bone Over Time
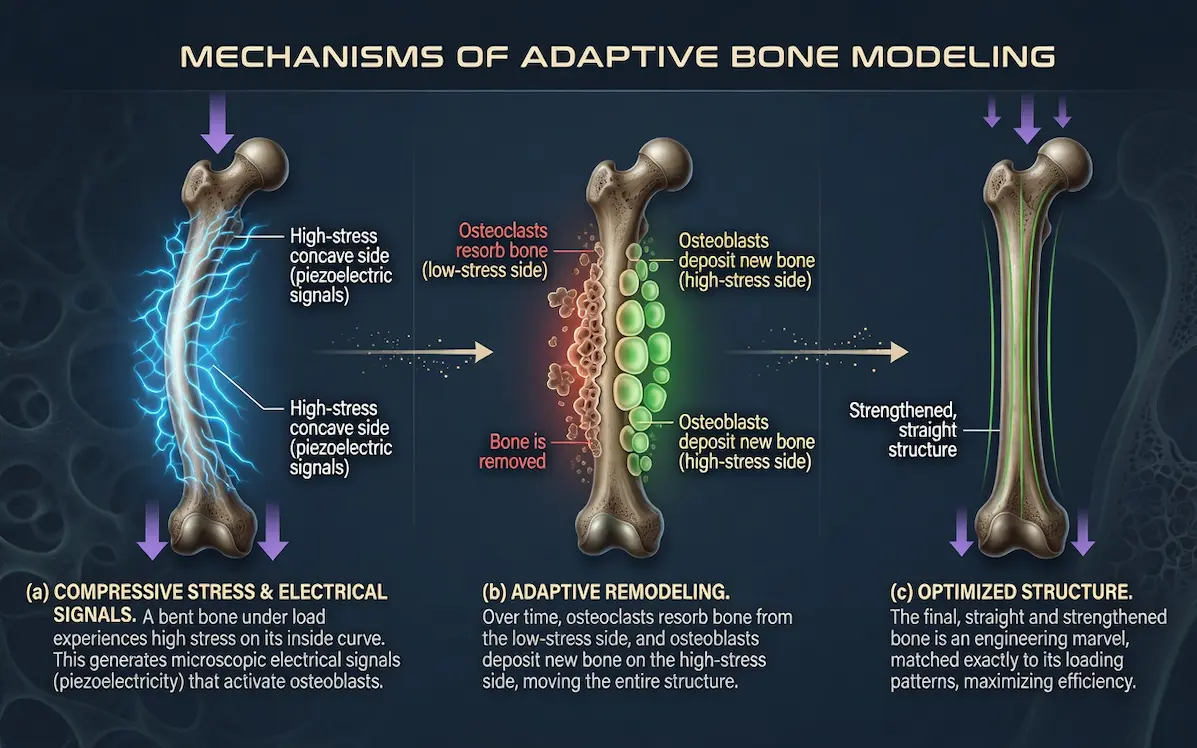
The clearest way to see how bone modeling works is to trace what happens when a consistently applied force acts on a slightly curved bone over an extended period.
The above sequence is one of the most instructive examples in bone biology, that shows both how bone changes and exactly why it changes the way it does.
This sequence illustrates the most important principle in bone modeling: bone does not change randomly.
It changes in a direction that matches its structure to the forces it experiences.
The concave side of a bent bone under compression experiences higher stress, osteocytes detect that stress and signal osteoblasts to reinforce it.
The convex side experiences lower stress, that signal is weaker, and osteoclasts are allowed to remove the excess.
Over months and years, the asymmetry resolves.[9]
The same logic applies to every other structural outcome of bone modeling.
The driving principle is always the same: bone builds where force demands it and retracts where force is absent.
What Types of Activity Drive Modeling?
Not all physical activity sends the same signal to bone.
The modeling response depends on the type, magnitude, and pattern of loading not just whether or not you are moving.
- High-impact loading like running, jumping, court sports, gymnastics produces strong modeling signals, particularly at the periosteal surface.[10]
This is the category of activity most consistently associated with increases in bone width and cortical thickness in the research literature.
- Directional loading; forces applied consistently in one orientation over time , drive modeling in that specific direction.
- Progressive loading:
This happens when mechanical load on bone is gradually increased to trigger the modeling process and with time, the bone adapts.
Once bone has adapted to a given load, that load no longer drives further modeling.
- Low-load repetitive activity:
Activities like casual walking, or light cycling can help to maintain the existing bone structure but do not reliably drive new modeling in healthy bone.
This is because the mechanical signal does not cross the threshold needed to upregulate osteoblast activity beyond maintenance levels.
How Modeling Contributes to Bone Length and Growth
Bone length increases through a separate mechanism called endochondral ossification which is a process driven by chondrocytes at the growth plates.
Modeling does not lengthen bone directly.
But it plays an essential role in how that lengthening process produces a functional, properly shaped bone structure.
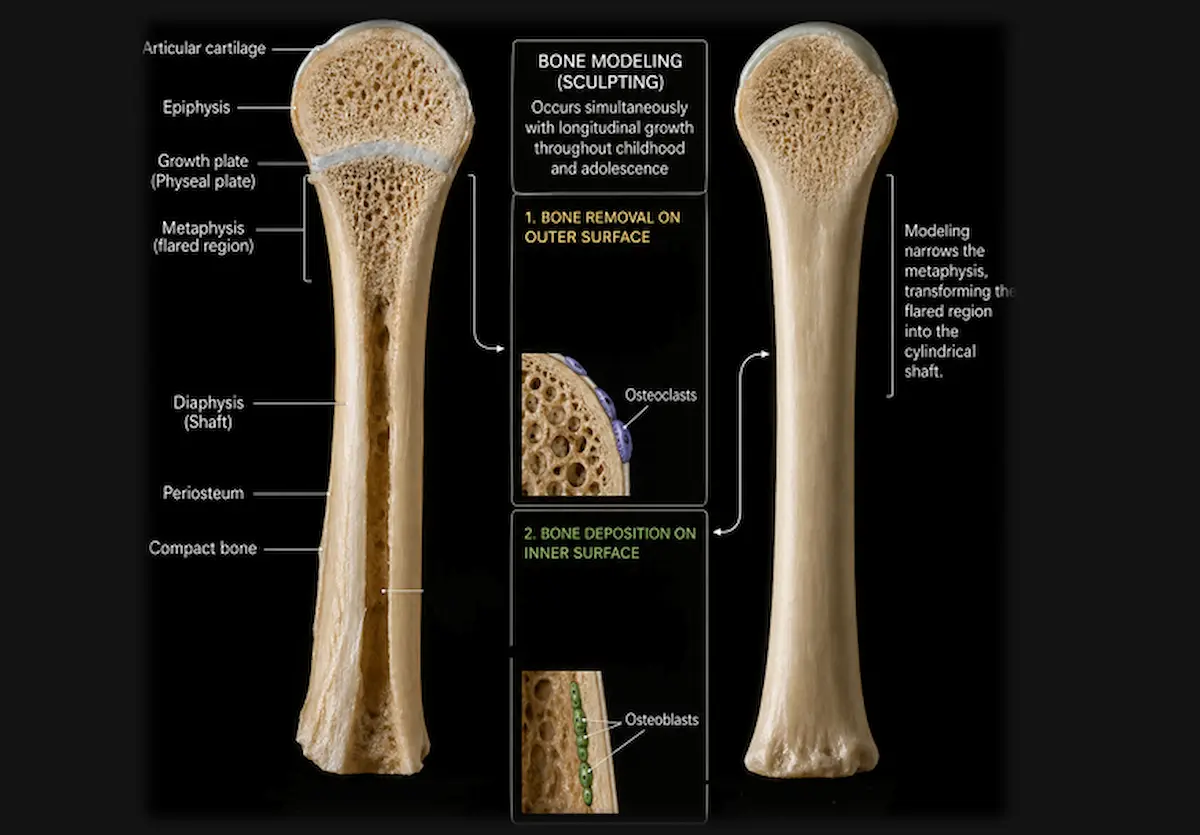
Sculpting the Bone as It Grows
As a long bone grows in length through the growth plate, the metaphysis which is the flared region just below the plate would become progressively wider and more distorted without concurrent modeling.
Osteoclasts remove bone from the outer periosteal surface of the metaphysis while osteoblasts deposit new bone on the inner endosteal surface, progressively narrowing the flare into the cylindrical shaft of the bone.[11]
This sculpting runs simultaneously with longitudinal growth throughout childhood and adolescence.
It is the reason growing bones maintain their proportions rather than becoming wider at the ends with each centimeter of length added.
Does Modeling Still Happen in Adults?
Yes. Bone modelling can still continue among adults especially in an adaptive response to mechanical loading and exercise or in the case of the renal bone disease.
The evidence for continued bone modeling in adults is not theoretical — it is measurable in imaging studies and consistently observed across different populations.[12]
Why It Slows With Age
Adult modeling is slower and more modest than adolescent modeling.
Declining hormonal signals, particularly growth hormone and sex hormones reduce the anabolic drive to the periosteum.
The osteocyte sensing network becomes less responsive.
And the osteoblast formation response takes longer to produce net bone gain.
None of this means modeling stops.
It means producing a meaningful structural response in adult bone requires more consistent, appropriate mechanical input and more time for that response to accumulate.
The practical implication:
Structural changes in adult bone develop over months to years of consistent loading, not weeks.
The mechanism is present.
The question is always whether the mechanical input is sufficient and sustained enough to drive it.
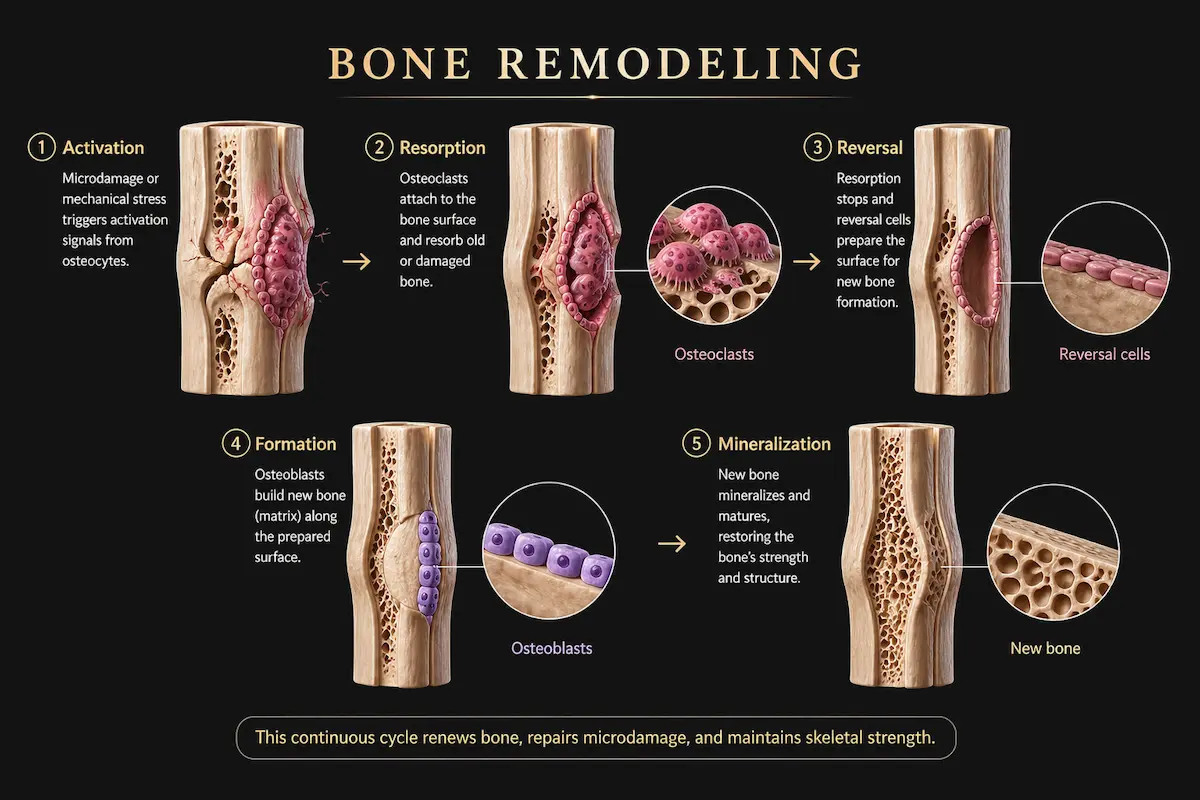
Bone Remodeling — How It Differs
Bone remodeling is frequently confused with bone modeling, and the two terms are often used interchangeably.
They describe different processes with different outcomes.
Bone remodeling replaces old or damaged bone with new bone in the same location, Osteoclasts act first then osteoblasts act sequentially at the same site, there’s no geometry change, and bone is renewed but shape is preserved.[13]
Remodeling matters because it is how the skeleton maintains its structural integrity over decades by replacing fatigued bone before microdamage accumulates into fracture. Roughly 5–10% of the adult skeleton is replaced through remodeling each year.
The healing of bone fractures is a perfect example of physiological bone remodeling because it demonstrates the body’s ability to not just repair damage, but to completely replace temporary, disorganized bone with mature, functional bone that adapts to mechanical stress.
Final thoughts
Bone modeling takes place behind the scenes on each and every physical activity day.
Continuously transforming the skeletal architecture in response to the external mechanical stimulus.
But most people never think of it that way.
References
1. Bone modeling and remodeling (2016)
2. Bone Matrix
3. The biology of normal bone remodeling (2017)
4. Osteoblast Differentiation and Bone Matrix Formation In Vivo and In Vitro (2017)
5. Role of osteoclasts in oral homeostasis and jawbone diseases (2020)
6. Mechanical regulation of bone remodeling (2022)
7. Mechanical Signaling for Bone Modeling and Remodeling (2009)
8. Periosteum and development of the tissue (2022)
9. Electric field stimulation-responsive hydrogels for bone regeneration (2026)
10.. Physical Activity and Bone Health (2014)
11. Metaphysis
12. The effect of exercise and nutrition on bone health (2018)
13. Physiology, Bone Remodeling (2023)
AUTHOR BIO

Dennis Raney (B.Sc.) is an author and a blogger specializing in natural body growth optimization strategies.
After years of navigating the psychological and physical challenges of being under-average height, Dennis dedicated over a decade to researching the intersection of lifestyle, nutrition, and body growth.
By applying an evidence-based approach to healthy lifestyle changes, he successfully navigated his own body transformation, an experience that led him to author his comprehensive guide on height increase during and after puberty.
Today, he shares practical, research-backed strategies through his book and blog to help others overcome similar challenges.”
Interested in connecting? :
✉️ Send an email: Dennis »»
💬 Add me on Discord: raney0029 »»